Stress Literacy – A Life is Biology Series
Stress Literacy is the ability to recognise how stress moves through the body before it becomes illness, burnout, or breakdown. This series treats stress not as emotion or mindset, but as a biological process; one that follows patterns, rhythms, and thresholds.
Each piece in this six-part sequence examines a distinct way stress disrupts recovery and regulation, often long before symptoms feel serious. The goal here is not to fix, optimise, or motivate, but to learn how to observe biological drift early, when intervention is still possible.
This first essay begins with the most common entry point: burnout – not as exhaustion, but as recovery that no longer restores.
Burnout is not how you feel.
You can feel motivated, disciplined, and even optimistic, and still be biologically burnt out.
Burnout does not begin as exhaustion.
It begins as something quieter:
recovery that no longer restores.
You can enjoy your work, believe in your mission, and maintain outward momentum — while your nervous system quietly shifts into survival mode.
Burnout is not an emotion.
It is a biological state.
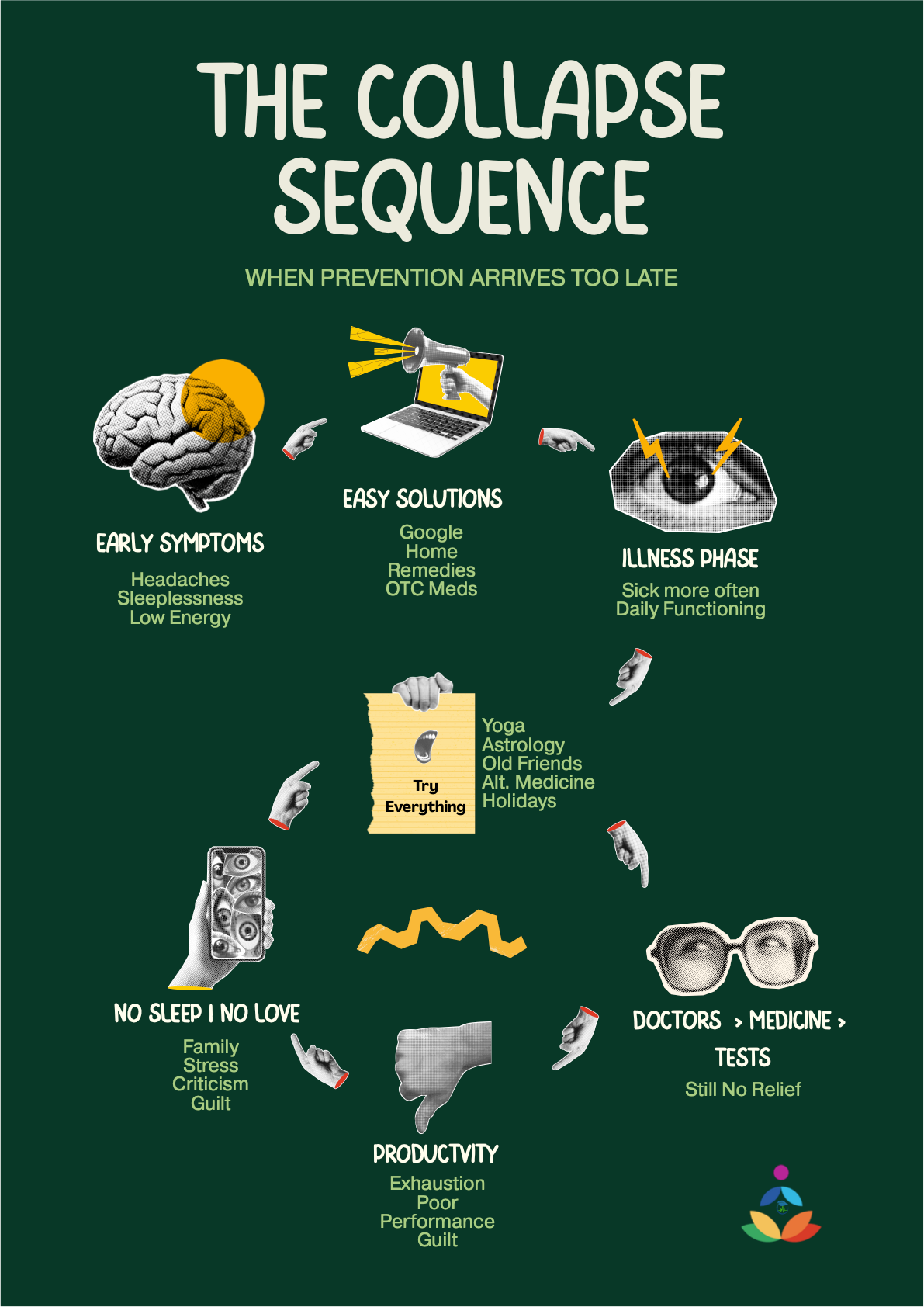
Most people imagine burnout as a mental crash.
But burnout rarely arrives that dramatically.
It begins quietly:
-
a morning where your body feels heavier than your plans,
-
sleep that doesn’t restore you,
-
a brain that won’t focus even though the calendar demands it,
-
irritability you justify as “just a long week.”
The truth is simpler and more sobering:
Burnout begins in the body long before the mind notices.
It is not a motivation problem.
It is not a productivity problem.It is a rhythm problem, a collapse in how your body restores itself.
This article explains burnout as a biological system failure, not a mindset issue, especially for entrepreneurs and high-responsibility professionals.
What follows blends psychology, physiology, HRV research, vagal theory, and new diagnostic tools (Lyfas + FSP-40) to build a clear model of how burnout forms, how it can be measured, and how recovery can be engineered.
Burnout as Rhythm Collapse, Not Stress Accumulation
The World Health Organisation formally recognised burnout in 2019 as an “occupational phenomenon” resulting from chronic workplace stress that has not been successfully managed (World Health Organisation, 2019).
But this definition misses the biological story.
Burnout is not simply “too much work” or “too many emotions.”
It is the loss of physiological recovery rhythms, the dynamic interplay of:
-
heart rate variability (HRV),
-
vagal tone,
-
hormonal cycles,
-
sleep quality,
-
metabolic and immune resilience.
Mental resilience narratives give the impression that burnout can be solved through mindset shifts, therapy, or lifestyle habits. While valuable, these interventions only address the emotional surface, not the biological core.
Stress leaves measurable signatures across the body weeks or months before collapse (McEwen, 2007). This means burnout is not only predictable, it is preventable.
To understand burnout, we must begin with biology.
What We Mean by Stress
Burnout is often described as emotional exhaustion or loss of motivation. In Stress Literacy, stress is defined differently. Stress is not an emotion, but a biological condition in which the body remains activated without sufficient recovery or return to baseline. Burnout represents the late stage of this process – the point where recovery no longer restores capacity. By the time burnout is felt, biological stress has already been present for a long time.
Stress as Biology, Not Just Psychology
When people say “I’m stressed,” they are usually describing a subjective state: anxiety, overwhelm, irritability, worry.
But stress is fundamentally a biological process, deeply rooted in the body’s regulatory systems.
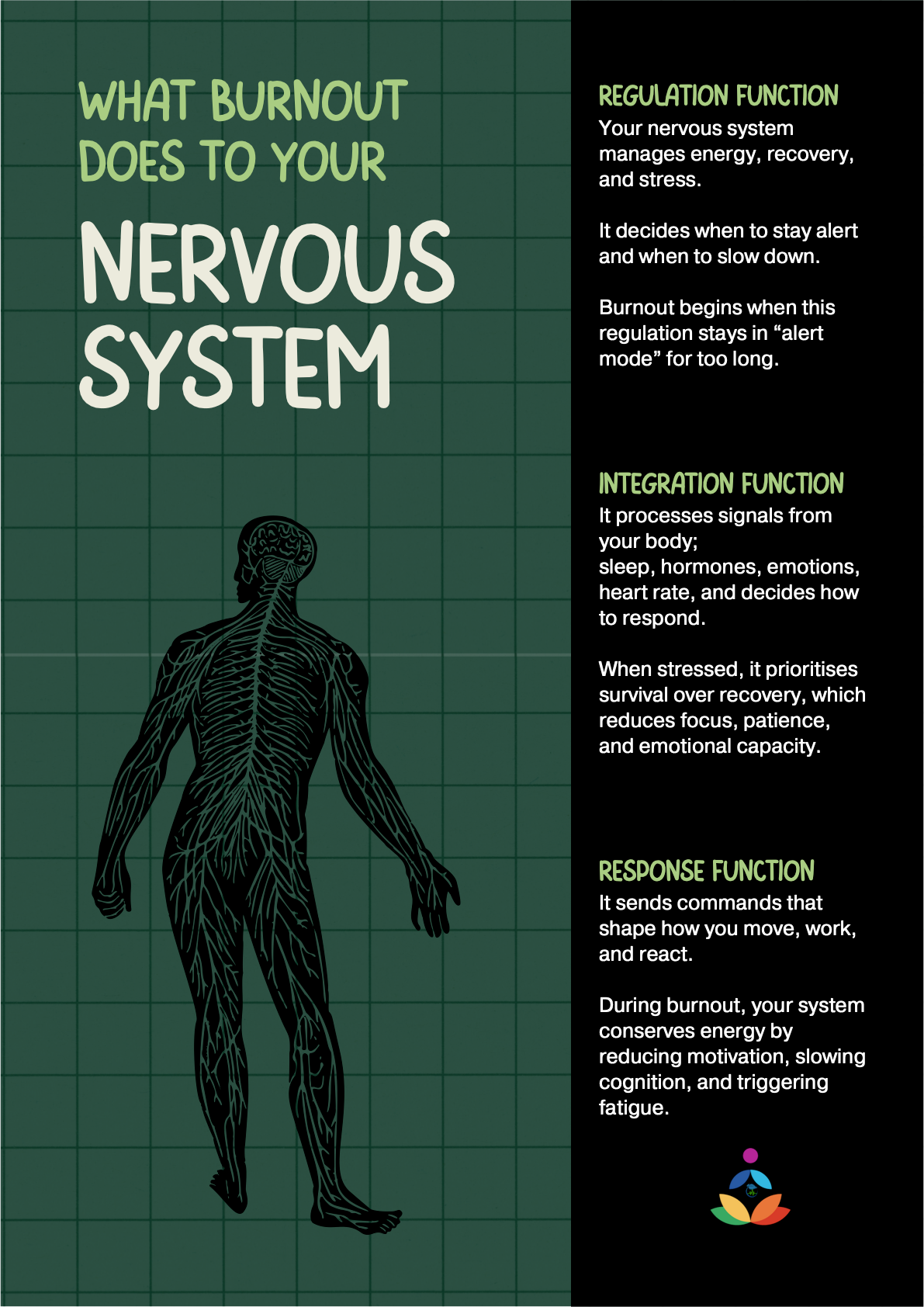
The Stress Response System
The autonomic nervous system (ANS) drives your stress response:
-
Sympathetic nervous system (SNS) – the accelerator (mobilising energy)
-
Parasympathetic nervous system (PNS) – the brake (restoring energy)
Healthy functioning requires rhythm; a smooth alternation between activation and recovery, often measured through HRV (Shaffer & Ginsberg, 2017).
Chronic stress destroys this rhythm.
The SNS stays activated.
The PNS goes offline.
Your system loses the ability to “come down.”
This imbalance dysregulates the HPA axis, driving prolonged cortisol exposure, impaired recovery, and what Bruce McEwen termed allostatic load – cumulative biological wear and tear (McEwen, 2007).
Biological Signatures of Chronic Stress
Stress creates measurable disruption in multiple systems:
Cardiac & Autonomic
-
Reduced HRV
-
Lower RMSSD
-
Flattened LF/HF ratio
Indicates loss of vagal regulation (Thayer & Lane, 2000).
Endocrine
-
Cortisol misalignment
-
Blunted diurnal rhythms
-
Poor recovery cycles (Miller et al., 2007)
Immune & Inflammation
Chronic stress elevates cytokines, increasing risk for cardiovascular and metabolic disorders (Black & Garbutt, 2002).
Cognitive & Emotional
Overactive amygdala, impaired prefrontal cortex regulation → reduced focus, poorer emotional control, anxiety (Arnsten, 2009).
None of this is “in your head.”
Burnout is the body’s biology failing to return to baseline.
Biology isn’t destiny but it responds only to signals, not intentions.
Why Founders Burn Out Faster and Differently
Entrepreneurs operate under conditions normal jobs never see:
-
asymmetric responsibility,
-
constant uncertainty,
-
identity entanglement (“I am my company”),
-
isolation in decision-making,
-
financial, emotional, and relational risk concentrated on one person.
A large-scale study by Michael Freeman et al. (2015) found:
-
72% of entrepreneurs report mental health concerns
-
far higher rates of depression, anxiety, and substance use than the general population.
But the deeper issue is not emotion, it is biology under load.
Functional Burnout
Founders specialise in masking distress.
They can keep performing externally while their internal systems fail silently:
-
sleep deteriorates,
-
HRV collapses,
-
vagal tone drops,
-
emotional range narrows,
-
energy becomes erratic.
Outward performance continues.
Internal recovery collapses.
This is why burnout in founders feels sudden.
Biologically, it wasn’t sudden at all.
The Founder Stress Pattern (FSP-40)
Your PDF explains this well. The six patterns map a multidimensional stress profile:
-
Cognitive Load (CL): decision fatigue, mental scattering
-
Execution Avoidance (EA): paralysis, procrastination
-
Emotional Suppression (ES): hiding vulnerability, constricted expression
-
Autonomic Reactivity (AR): shallow breath, palpitations, body agitation
-
Chronic Burnout (CB): exhaustion, sleep dysfunction, emotional drainage
-
Existential Tension (ET): identity collapse, meaning erosion
These are not personality traits.
They are physiological consequences.
The Missing Metric: Recovery Capacity
Healthcare systems detect illness, not collapse.
Blood reports and scans catch pathology, not rhythm.
A founder may have:
-
normal LDL,
-
normal thyroid,
-
normal sugar,
-
normal vitamin markers…
…and still operate with:
-
suppressed HRV,
-
dysfunctional sleep,
-
chronic sympathetic dominance,
-
emotional flatness.
Wearables help but fall short:
-
fragmented metrics,
-
inconsistent use,
-
lack of interpretation (Patel et al., 2015).
What founders need is clarity, not dashboards.
Recovery is the missing metric.
Best measured through:
-
HRV
-
RSA (respiratory sinus arrhythmia)
-
Cortisol slope
-
Vagal tone indicators
These show adaptability versus collapse (Shaffer & Ginsberg, 2017; Miller et al., 2007).
Check-INS vs Check-UPS
Check-up → pathology, occasional, reactive
Check-in → rhythm, frequent, preventive
Lyfas + FSP-40 creates this integrated model:
-
subjective stress expression,
-
objective biology,
-
actionable recovery direction.
Performance Is Biological (Not Motivational)
The opposite of burnout is not “relaxation.”
It is capacity, the ability of your body to restore energy faster than you spend it.
Elite Performance Principles
Athletes train by HRV.
Founders work by calendar.
One optimises biology; the other ignores it (Stanley et al., 2013).
Sleep is active recovery.
Slow-wave sleep restores immune function.
REM sleep stabilises emotion (Walker, 2017).
Stress disrupts both, producing “non-restorative sleep” (Trinder et al., 2001).
Vagal Tone = Better Decisions
High vagal tone → better emotional regulation, focus, clarity (Arnsten, 2009; Lehrer & Gevirtz, 2014).
Recovery is not rest.
Recovery is system repair.
Conclusion
If burnout were a feeling, reassurance would solve it.
But burnout is biological.
And biology responds only to rhythm, load, recovery, and signal quality,
not intention, motivation, or belief.
Before changing habits, optimising performance, or searching for meaning, start here:
observe energy before emotion.
Burnout does not begin when you feel exhausted.
It begins when recovery no longer restores.
That is the signal this series is designed to help you recognise.
What blocks recovery and why, comes next.
References
American Institute of Stress. (2019). Workplace stress statistics. Retrieved from https://www.stress.org/workplace-stress
Arnsten, A. F. T. (2009). Stress signalling pathways that impair prefrontal cortex structure and function. Nature Reviews Neuroscience, 10(6), 410–422.
Black, P. H., & Garbutt, L. D. (2002). Stress, inflammation and cardiovascular disease. Journal of Psychosomatic Research, 52(1), 1–23.
Boyes, A. (2020). The anxiety toolkit: Strategies for fine-tuning your mind and moving past your stuck points. HarperOne.
Cohen, S., Kamarck, T., & Mermelstein, R. (1983). A global measure of perceived stress. Journal of Health and Social Behavior, 24(4), 385–396.
Das, R. (2021). Smartphone-based photoplethysmography for stress and HRV monitoring: Clinical validation of Lyfas. European Society of Medicine Proceedings.
Freeman, M. A., Staudenmaier, P. J., Zisser, M., & Andresen, L. A. (2015). The prevalence and co-occurrence of psychiatric conditions among entrepreneurs and their families. Small Business Economics, 45(3), 563–574.
Gross, J. J. (1998). The emerging field of emotion regulation: An integrative review. Review of General Psychology, 2(3), 271–299.
Juneja, L. R., Chu, D. C., Okubo, T., Nagato, Y., & Yokogoshi, H. (1999). L-theanine—a unique amino acid of green tea and its relaxation effect in humans. Trends in Food Science & Technology, 10(6–7), 199–204.
Kennedy, D. O., Wightman, E. L., & Reay, J. L. (2014). Herbal extracts and brain function: Evidence for modulation of mood and cognition. Neurochemistry International, 64, 57–71.
Lehrer, P., & Gevirtz, R. (2014). Heart rate variability biofeedback: How and why does it work? Frontiers in Psychology, 5, 756.
Levenstein, S., Prantera, C., Varvo, V., Scribano, M. L., Berto, E., Luzi, C., & Andreoli, A. (1993). Development of the Perceived Stress Questionnaire: A new tool for psychosomatic research. Journal of Psychosomatic Research, 37(1), 19–32.
Lovibond, S. H., & Lovibond, P. F. (1995). Manual for the Depression Anxiety Stress Scales. Psychology Foundation of Australia.
Maslach, C., & Leiter, M. P. (2016). Understanding the burnout experience: Recent research and its implications for psychiatry. World Psychiatry, 15(2), 103–111.
McEwen, B. S. (2007). Physiology and neurobiology of stress and adaptation: Central role of the brain. Physiological Reviews, 87(3), 873–904.
McEwen, B. S., & Stellar, E. (1993). Stress and the individual: Mechanisms leading to disease. Archives of Internal Medicine, 153(18), 2093–2101.
McKay, D. L., Chen, C. O., Saltzman, E., & Blumberg, J. B. (2010). Hibiscus sabdariffa L. tea (tisane) lowers blood pressure in prehypertensive and mildly hypertensive adults. Journal of Nutrition, 140(2), 298–303.
Miller, G. E., Chen, E., & Zhou, E. S. (2007). If it goes up, must it come down? Chronic stress and the hypothalamic–pituitary–adrenocortical axis in humans. Psychological Bulletin, 133(1), 25–45.
Pascoe, M. C., Thompson, D. R., Jenkins, Z. M., & Ski, C. F. (2017). Yoga, mindfulness-based stress reduction and stress-related physiological measures: A meta-analysis. Psychoneuroendocrinology, 86, 152–168.
Patel, M. S., Asch, D. A., & Volpp, K. G. (2015). Wearable devices as facilitators, not drivers, of health behavior change. JAMA, 313(5), 459–460.
Porges, S. W. (2007). The polyvagal perspective. Biological Psychology, 74(2), 116–143.
Shaffer, F., & Ginsberg, J. P. (2017). An overview of heart rate variability metrics and norms. Frontiers in Public Health, 5, 258.
Shahid, A., Wilkinson, K., Marcu, S., & Shapiro, C. M. (2012). STOP, THAT and one hundred other sleep scales. Springer Science+Business Media.
Stanley, J., Peake, J. M., & Buchheit, M. (2013). Cardiac parasympathetic reactivation following exercise: Implications for training prescription. Sports Medicine, 43(12), 1259–1277.
Thayer, J. F., & Lane, R. D. (2000). A model of neurovisceral integration in emotion regulation and dysregulation. Journal of Affective Disorders, 61(3), 201–216.
Trauer, J. M., Qian, M. Y., Doyle, J. S., Rajaratnam, S. M., & Cunnington, D. (2015). Cognitive behavioral therapy for chronic insomnia: A systematic review and meta-analysis. Annals of Internal Medicine, 163(3), 191–204.
Trinder, J., Allen, N., Kleiman, J., & Kralevski, V. (2001). Autonomic activity during human sleep as a function of time and sleep stage. Journal of Sleep Research, 10(4), 253–264.
Walker, M. (2017). Why we sleep: Unlocking the power of sleep and dreams. Scribner.
World Health Organization. (2019). Burn-out an “occupational phenomenon”: International Classification of Diseases. Retrieved from
Zaccaro, A., Piarulli, A., Laurino, M., Garbella, E., Menicucci, D., Neri, B., & Gemignani, A. (2018). How breath-control can change your life: A systematic review on psychophysiological correlates of slow breathing. Frontiers in Human Neuroscience, 12, 353.